What is Chinese Medicine?
Chinese medicine is one of the oldest medical systems which determines patterns of disharmony to balance through subjective and objective findings, such as palpation, tongue and pulse diagnosis.
Chinese Medical Diagnostics
Chinese Medicine (CM) utilizes several diagnostic systems of differentiation which are combined in clinical practice to confirm that the diagnosis and subsequent treatment is sound. The most basic diagnostic parameter is yin and yang. This is expanded upon by defining excess or deficiency. Another common system is called zangfu, where one or two organs are defined, as well as a quality, such as Liver qi stagnation, or Spleen qi deficiency. This can be likened to a congested liver, or the insufficient transformation of our food due to poor enzyme output.
- Yin
- Interior
- Cold
- Deficient
- Yang
- Exterior
- Hot
- Excessive
- YIN
- Anterior aspect of the body
- Chronic conditions
- Solid organs: storage: pure essences, vital substances (qi, blood, shen, jing)
- Blood and fluids
- Underactive
- Lethargic
- Fatigue
- Cold/cool
- Lack of thirst
- Dampness
- Pale
- Tongue – pale
- Pulse – Empty
- YANG
- Posterior aspect of the body
- Acute conditions
- Hollow organs – no storage: transforms, digests and eliminates impurities (urine, fecal matter)
- Qi
- Overactive
- Restless
- Insomnia (excess type)
- Hot/warm
- Thirst
- Dryness
- Red
- Tongue – Red
- Pulse – Full
- DEFICIENCY PATTERNS
- Qi Deficiency
Fatigue, loose stools, poor appetite, dizziness, pale face, weak voice/reluctance to speak, easy sweat
Tongue – Pale
Pulse – Empty
- Yang Deficiency
Chills, cold limbs, inability to get warm, loose stools, profuse clear urine, spontaneous sweating, lassitude
Tongue – Pale with a white coating
Pulse – Slow, deep, weak
- Yin Deficiency
Heat in the hands, feet or chest, malor flush, night sweats, anxiety, hot flashes
Tongue – red with little or no coat
Pulse – Thin, rapid
- Blood Deficiency
Dizziness, palpitations, insomnia, dry skin and/or hair, poor memory, paleness, fatigue, scanty periods
Tongue – Pale, thin, dry
Pulse – Thin, choppy
- EXCESS PATTERNS
- Qi Stagnation
Distention – such as abdominal, breast; pains that move around, depression, irritability
Tongue – Purple
Pulse – Wiry
- Heat (Excess Yang)
Agitation, anger, insomnia with nightmares, fever, red face/head, constipation, desire for cold drinks
Tongue – Red, dry with yellow coat
Pulse – Rapid, full
- Cold (Excess Yin)
Chills without sweating, lack of thirst, clear urine, aversion to cold, loose stools, fatigue
Tongue – Pale with white coat
Pulse – Slow, deep, tight
- Blood Stagnation
Pain that is fixed, stabbing and/or severe, dark complexion, fixed masses, bleeding with clots, purple lips/nails
Tongue – Purple
Pulse – Wiry, choppy
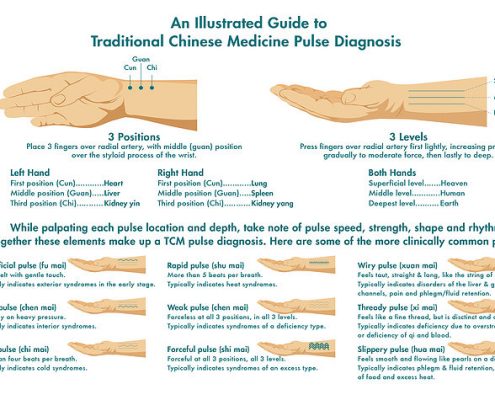
Pulse and tongue diagnosis are important diagnostic tools.
The pulse is palpated at the radial artery to sense it’s depth, frequency, quality, shape, length, width, strength, and rhythm. One example of a pulse type is a floating pulse. The pulse will raise to the surface when the body is fighting an acute attack (infection). Just like sending the troops to the front lines. Your body is attempting to ward off deeper invasion.
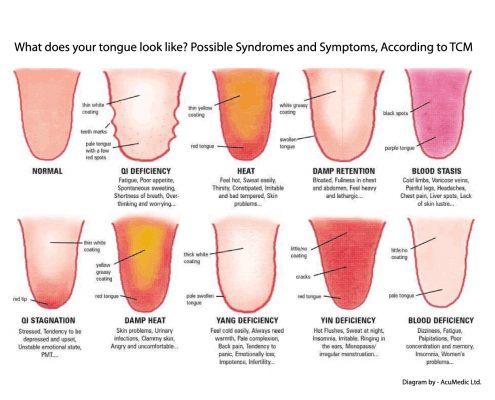
The tongue is a diagnostic muscle that we can easily see. It is assessed by its tonicity, shape, color, and coating. A swollen tongue that has teeth marks along it’s periphery, is from the retention of water. Whereas a thin tongue may be from anemia or dehydration. Its geography is also mapped by the meridians.
PULSE DIAGNOSIS
The pulse has three positions and three depths. It not only provides the rate, but also a quality. If the position associated with the lower segment of the body is stronger than the middle and upper segments, it implies that something is going on near the pelvic region. Ideally the pulse will be balanced between it’s three positions, and three levels.
TONGUE DIAGNOSIS
The tongue is assessed by its tone, color and coating. A healthy tongue would be light red, not too flaccid, not too rigid, with a thin white coating. A rigid tongue can be a sign of stagnation or heat cooking off the fluids. If it is flaccid, it is a sign of depletion, or weakness. If your body is very dry, your tongue may look red and firm, or have lots of cracks. If is full of fluid, it will look swollen and wet. The coating provides a lot of information about what is happening in your stomach. A thick coating implies that your food is not transforming well. A lack of coating implies that your stomach is too dry.
Chinese Pattern Differential
Traditional Chinese Medicine combines the patient’s detailed history, a thorough subjective questionnaire, a physical examination, include tongue and pulse assessment, to determine the patient’s pattern of disharmony.
Example:
Patient complains of stomach bloating and pain, and diarrhea. Her bloating and stomach pain are worse after drinking an ice coffee, or eating a salad. Her pain can sometimes be extreme, and only finds relief by lying in the fetal position. Sometimes she see food particles in her stools. She also has urgency.
Palpation: Her abdomen is cold
Tongue: Thick white coating
Pulse: Deep, slow and tight
Diagnosis: Cold in the stomach causing stagnation
Treatment: Avoid cold drinks and foods. Cook foods. Far infrared, moxa, and/or massage to the abdomen. An herbal formulation that warms and regulates the digestion.
Lets use the same symptoms, but a different presentation:
Patient complains of stomach bloating and pain, and diarrhea. Her stomach bloating and pain are worse after eating bread or having desert, and often causes nausea. Her diarrhea is slightly sticky.
Palpation: No notable temperature variance. Notable epigastric stagnation with aversion to pressure
Tongue: Body is puffy, with a thick white coating
Pulse: Slippery
Diagnosis: Damp accumulation in the middle (Stomach and Spleen)
Treatment: Drain dampness, regulate the middle
Chinese Medicine vs. Functional Medicine
Chinese Medicine and Functional Medicine are similar in the sense that both are working to improve health, versus manage disease. They both personalize their treatments to the individual patient, versus a one-size-fits all approach. And both emphasis diet and lifestyle for treatment success.
Functional medicine utilizes diagnostic testing to determine physiologic function. Treatment is based on the testing results, and botanical therapies are preferred. The treatment recommendations often reflect the practitioners background. An MD will utilize pharmaceuticals such as Tidamax for a parasite, whereas a Chiropractor or Naturopath will utilize botanicals, but in a green pharmacy format, a this-for-that principle. For example – if you have a positive SIBO breath test, you will be treated with botanicals that are know to treat SIBO, without much thought of your physiology and how you will react to the recommended botanicals.
Chinese Medical Practitioners do not have diagnostic testing, and must rely of the patient’s subjective input, and the practitioners objective assessment.
Chinese Medicine & Functional Medicine
I feel the best practitioner to work with is a Chinese Medical Practitioner that is also trained in Functional medicine.
You would be provided with detailed, personalized recommendations as it pertains to diet and lifestyle. Diagnostic testing interpretation with treatment recommendations, but these botanical recommendations would be prescribed with your physiology in mind, based on Chinese medical assessments. If some of the diagnostic testing cannot be obtained, due to access or cost, a treatment plan can still be created based on Chinese medical analysis.